Root canal therapy has three purposes
- Stop the toothache
- Prevent bacteria and pain from spreading into the jaw
- Maintain the original tooth instead of replacing it with a denture or bridge.
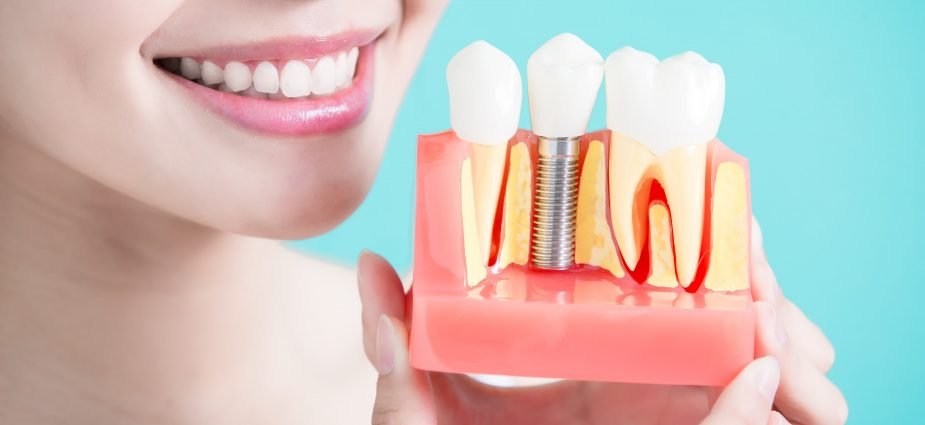
The root canal is actually a channel that runs from the root of the tooth, to the top surface of the tooth, and connects it to the bone. The canal contains blood vessels, nerves, and the complex cells that make up the living tissue inside the tooth. This is called the pulp.
When a tooth is decayed or cracked, bacteria can get to the pulp. The acid from the bacteria irritates the pulp and it becomes inflamed; it’s the same process you watch when other parts of your body become infected. When the pulp tissue becomes inflamed, it’s harder for blood to flow to the tissue, and the resulting pressure creates pain inside your tooth.
There are two ways to get relief from the pain: perform the root canal therapy, or pull the tooth, clean the gum below, and replace the tooth with a denture or bridge. Dentists advise pulling teeth as a last resort because they know that your natural teeth are the ones best suited for your mouth.
It’s important to have root canal therapy done quickly. The bacteria will travel down the canal to the root and into the jawbone. If this happens, the pain of your toothache will spread to your jaw. Even more important, the infection can cause your jawbone to deteriorate and weaken the structure that holds your teeth.
The best way to avoid root canals is to take good daily care of your teeth to prevent the growth and spread of bacteria. Brushing and flossing are important. Just as important are regular trips to the dentist, to check for the first sign of decay or cracks that could eventually lead to an infected tooth. In this case, an ounce of prevention really is worth a pound of cure!
What Is the Cost of Root Canal Treatment?
There are many factors that affect the cost of root canal treatment. Each patient and tooth presents a different set of circumstances. Generally, the cost of root canal treatment is directly related to the chair time necessary to perform the treatment as well as to the costs of the staff, training, and technology that the dentist has available when performing the procedure. There are many factors that influence the amount of chair time necessary to treat any particular tooth:
- The position of the tooth in the mouth
- The number of roots and the number of canals within these roots
- Root curvatures and the length of the roots
- The presence or absence of calcifications within the root canal space
- Special dental considerations. For example, it may be more difficult for the dentist to work through an existing crown or a bridge than to work on a tooth with only a small previous filling. Also, some teeth may have been severely broken down by past dental disease and these may have to be “built-up” before root canal treatment can even be started so that an aseptic field can be established and maintained during treatment.
In addition to the chair time involved for treatment, other factors are also taken into consideration when determining a fair fee for root canal treatment:
- The cost of technology. Dentists who use state-of-the-art technology for certain procedures have invested in computer digital radiography, ultrasonic, and specialized training courses for themselves and for their staff. Those patients who benefit from them share the costs of these items.
- The costs of the dental office overhead include staff, rent, and supplies in addition to many other expenses. These costs vary significantly in different areas of the country.
- Fees vary among practitioners due to differences in their endodontic treatment philosophies, which in turn dictate the chair time required, the materials selected, and the technologies utilized.
In conclusion, there can be marked discrepancies in the fees charged for root canal treatment by different dentists. Ultimately, the best value for care is treatment that is done once and works over a period of many years. Conversely, the most expensive dental treatment is the treatment that may cost less initially but does not work predictably and needs to be redone one or more times. The wise dental consumer does not make a treatment decision on the basis of cost alone.
The Root Reasons For A Root Canal – Many people flinch when their dentists tell them they need root canal therapy. While dentists are sympathetic to fears of pain,
Dental Health: Symptoms Of Endodontic Disease
What Are the Most Common Symptoms of Endodontic Disease?
Endodontic disease can manifest itself with a wide variety and combination of symptoms. Common symptoms of endodontic disease include:
- Lingering tooth sensitivity to cold liquids.
- Lingering tooth sensitivity to hot liquids.
- Tooth sensitivity to sweets.
- Tooth pain to biting pressure.
- Tooth pain that is referred from a tooth to another area, such as the neck, temple, or the ear.
- Spontaneous toothache, such as that experienced while reading a magazine, watching television, etc.
- Constant or intermittent tooth pain.
- Severe tooth pain.
- Throbbing tooth pain.
- Tooth pain that may occur in response to atmospheric pressure changes, such as when flying or scuba diving.
- Tooth pain that may occur in response to postural changes, such as when going from a standing to a reclining position.
- Tooth Swelling.
If you have any of these symptoms, it would be wise to see your dentist because you might have root canal disease or another dental problem. Some of these symptoms may also be attributable to decay, defective fillings, periodontal diseases, cracked teeth, or other tooth or bite-related problems. On other occasions, the symptoms may even be caused by disorders that are not related to the teeth.
Why May Endodontic Disease Cause Swelling?
When the pulp tissue becomes severely diseased and necrotic, the resultant infection can spread from inside the tooth into the adjacent bone and soft tissues. As a result, swelling can occur in the tissues immediately surrounding the tooth. If this situation is not treated and the disease process is not kept under control by the body’s defences, the infection can begin to spread into other tissue spaces, such as those around the eye or in the neck. In some situations, this can become a serious medical emergency.
Root Canal Retreatment
Can an Endodontically Failing Tooth Be Retreated?
Even when pain and/or swelling is present, the majority of failing endodontically-treated teeth can be successfully retreated in today’s world of clinical possibility. By using scientific information gathered from research and clinical studies, clinicians have developed better endodontic concepts, materials, and techniques. Additionally, there are now better-trained general dentists and specialists alike. All of these factors translate into improved care for patients. The significant technological breakthroughs that benefit both doctors and patients in endodontic retreatment include:
- Magnification glasses, fibre optic lighting sources, headlamps, have significantly improved vision and hence elevated treatment success.
- Ultrasonic devices allow doctors to more efficiently and completely remove old root canal filling materials and other intra-canal obstructions so that teeth may be successfully retreated.
- Computer digital radiography technology allows the doctor to better diagnose, visualize, and treat root canal disease. Additionally, this technology significantly reduces radiation exposure to the patient.
- Improved instruments, better materials for filling and repairing canals, and innovative new technologies have all contributed to significantly improved retreatment success.
Today, well-trained general dentists and specialists alike can oftentimes perform non-surgical endodontic retreatment in a very predictable, cost-effective, and time saving manner when compared to other treatment alternatives. At times, however, retreatment cannot be managed with non-surgical efforts alone. In these situations, and as an alternative to extraction, a surgical approach may be necessary.
What Is Non-Surgical Root Canal Treatment (NSRCT)?
Non-surgical root canal treatment is a procedure directed towards saving an endodontically failing tooth. At times, the patient’s existing artificial crown must be removed. In other instances, access through the crown may be possible. The access opening is created in order to give the dentist non-surgical access into the root canal space through the biting surface of the tooth. Once this has been accomplished, a non-surgical retreatment procedure oftentimes requires:
- Locating and treating previously missed canals.
- Removing old filling materials from the root canal space.
- Removing posts and broken instruments.
- Enhancing existing root canal treatment.
- Negotiating blocked canals and bypassing canal ledges.
- Repairing mechanical and pathological perforations in the root.
Once these objectives have been accomplished, the root canal system is re-cleaned, re-shaped, disinfected, and three-dimensionally sealed. A protective restoration can then be placed and the tooth restored to a state of health and function.
What Is Surgical Root Canal Treatment (SRCT)?
Surgical root canal treatment is a procedural effort in which it is necessary to elevate a small flap of tissue adjacent to the involved tooth in order to gain access to and treat root canal disease. Surgical root canal treatments are usually minor, in-office procedures performed under local anaesthesia. Once the pathological area is exposed, the doctor performs a “curettage” to remove the diseased tissue from around the root. This is usually followed by an “apicoectomy,” a procedure in which the diseased portion of the root is removed. A small filling is then usually placed to seal the remaining portion of the root. Surgical root canal treatment will oftentimes result in a good long-term prognosis for the tooth if the cause of pathology can be effectively eliminated.
Unfortunately, on occasion, retreatment efforts may not be possible or cost-effective and extraction may be the only alternative. However, saving a tooth that has been previously treated endodontically and is failing is usually possible, can be very predictable, and is typically the most conservative option for the patient.
Facts About Root Canal Treatment
What Are the Goals of Root Canal Treatment?
As an alternative to an extraction, the goals of root canal treatment are to save the tooth and allow it to be retained in the mouth for many years in a state of health, function, and comfort. Root canal treatment is directed towards removing diseased tissue from the inside of the tooth and subsequently filling and sealing the root canal space in order to minimize the possibility of future re-infection.
Why Is Root Canal Treatment Called Endodontic Treatment?
Endodontic is a word composed of two Greek words, “endo” meaning “inside,” and “odont” meaning “tooth.” Endodontics is that branch of dentistry that deals with the diagnosis, prevention, and treatment of diseases that arise from the soft tissues inside the tooth. These tissues are referred to as the dental pulp and they occupy the root canal space. Thus, endodontic treatment is also called root canal treatment.
If a Tooth Has Had Root Canal Treatment, Is It a Dead Tooth?
Root canal treatment does not kill a tooth. Even though root canal treatment removes the pulp tissue from inside the tooth, the tooth is by no means “dead.” Following successful endodontic treatment, the tooth continues to receive its blood supply and nourishment from the surrounding tissues and the supporting bone. The body’s immune system continues to recognize an endodontically treated tooth as viable and healthy, just as it recognizes any other normal non-treated tooth. An endodontically treated tooth generally requires a protective crown and, once this restoration has been completed, the tooth continues to function as an integral component of the dental arch. A tooth that has had root canal treatment and has been properly restored is no more susceptible to fracture, decay, or gum disease than any other tooth.
Alternatives To Root Canal Treatment
The only alternative to root canal treatment is the extraction of the problematic tooth. It is wise to consider all of the implications of losing a tooth before having it removed. The decision should not be made hastily or because the tooth is painful. If pain is present and the dentist thinks that the tooth can be saved, the discomfort can first be relieved and then the alternatives explored.
The discussion about tooth replacement alternatives after extraction can be complex because each individual situation is unique and, at times, various specialists may need to be consulted. When considering the alternatives for replacing a missing tooth, a few of the major factors to consider are the long-term predictabilities of the various alternatives, the overall chair time involved in treatment, the esthetic results, the effects on the adjacent and opposing teeth, and the costs. The usual alternatives that a patient has after tooth extraction are:
- A restored dental implant. This restoration involves a surgical procedure to insert the dental implant into the bone, a healing phase of several months, and a final restorative phase, which is similar to having a single tooth crown. Significant time and laboratory costs are involved.
- A fixed bridge. Fabricating a fixed bridge requires cutting down (“preparing”) the teeth next to the missing tooth so that they can receive the artificial crowns that support the replacement tooth. These teeth must be strong and healthy if they are to be effective bridge supports. Preparing the teeth for crowns could have a detrimental effect on their pulp health, depending on a variety of factors. This possibility needs to be discussed and factored into your decision. Fixed bridges may take multiple appointments to complete and have significant associated costs.
- A removable partial dentures. These appliances restore function and esthetics and can be inserted into the mouth and removed at will. Although many teeth are successfully replaced with removable prosthetic appliances, patients may initially find them cumbersome. Removable partial dentures may also temporarily alter phonetics as well as place unfavourable forces on the supporting teeth and soft tissues. There may be significant costs associated with this restoration.
- Not replacing the extracted tooth. This is a poor choice in most situations. Leaving a space after extraction can lead to long-term problems with teeth shifting and tipping, destabilization of the biting system, and esthetic changes in the profile of the face. Financially and psychologically, this could turn out to be the most costly choice over the lifetime of the patient.
After considering and weighing all of the consequences of extraction and all of the alternatives for tooth replacement, in most situations it becomes obvious that well-performed root canal treatment with a protective restoration is the treatment of choice. .